Hemorrhoids [piles]
- Home
- Health Topics:
- Hemorrhoids [piles]
Hemorrhoids (HEM-uh-roids), also called piles, are swollen and inflamed veins in your anus and lower rectum. Hemorrhoids may result from straining during bowel movements or from the increased pressure on these veins during pregnancy, among other causes. Hemorrhoids may be located inside the rectum (internal hemorrhoids), or they may develop under the skin around the anus (external hemorrhoids).
Hemorrhoids are common ailments. By age 50, about half of adults have had to deal with the itching, discomfort and bleeding that can signal the presence of hemorrhoids.
Fortunately, many effective options are available to treat hemorrhoids. Most people can get relief from symptoms by using home treatments and making lifestyle changes.
What Are Hemorrhoids?
They’re swollen blood vessels of the rectum. The hemorrhoidal veins are located in the lowest area of the rectum and the anus. Sometimes they swell so that the vein walls become stretched, thin, and irritated when you have bowel movements.
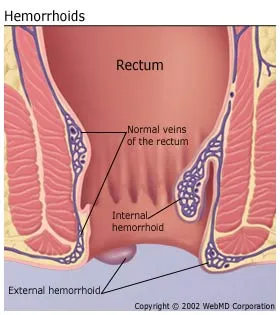
Are Yours Internal or External?
Internal hemorrhoids lie far enough inside the rectum that you can’t see or feel them. They don’t usually hurt because there are few pain-sensing nerves in the rectum. Bleeding may be the only sign they’re there.
Sometimes internal hemorrhoids “prolapse,” or enlarge and protrude outside the anal sphincter. When this happens, you may be able to see or feel them as moist, pink pads of skin that are pinker than the surrounding area. Prolapsed hemorrhoids may hurt because the anus is dense with pain-sensing nerves. They usually go back into the rectum on their own. If they don’t, they can often be gently pushed back into place.External hemorrhoids lie within the anus. They’re usually painful. If they move, or prolapse, to the outside (usually when you have a bowel movement), you can see and feel it.
Blood clots sometimes form within prolapsed external hemorrhoids, causing a very painful condition called a thrombosis. If that happens, the hemorrhoid can turn purple or blue, and could possibly bleed. Despite its appearance, it’s usually not serious, apart from the pain. It will go away in a couple of weeks. Your doctor can remove it if the pain is unbearable.
You should get any anal bleeding and pain checked by a doctor to make sure it’s not a more serious condition. Hemorrhoids are the No. 1 cause of this type of bleeding and are rarely dangerous, but you should find out for sure.
What Causes Them?
Doctors don’t know the exact cause. Some people may be more likely to get them because they have “weak” veins, leading to hemorrhoids and other varicose veins. That may be something you inherit.
There are other possibilities, too. It’s likely that extreme abdominal pressure makes the veins swell and become likelier to get irritated. The pressure can be caused by:
- Obesity
- Pregnancy
- Standing or sitting for a long time
- Straining during bowel movements
- Coughing
- Sneezing
- Vomiting
- Holding your breath when you do something that’s physically hard
What Are Hemorrhoids?
Hemorrhoids are swollen veins located around the anus or in the lower rectum. The Mayo Clinic reports that about half of adults have experienced the symptoms of hemorrhoids by the age of 50.
Hemorrhoids can either be internal or external. Internal hemorrhoids develop within the anus or rectum. External hemorrhoids develop outside of the anus. Hemorrhoids are also known as piles.
Of the two forms of hemorrhoids, external hemorrhoids are the most common and the most troublesome. Hemorrhoids cause pain, severe itching, and difficulty sitting. The good news is that they’re treatable.
What Are the Symptoms of Hemorrhoids?The symptoms of hemorrhoids include:
- extreme itching around the anus
- irritation and pain around the anus
- an itchy or painful lump or swelling near your anus
- fecal leakage
- a painful bowel movement
- blood on your tissue after having a bowel movement
Although hemorrhoids are painful, they aren’t life-threatening and often go away on their own without treatment. If you have them often, you may develop symptoms of anemia such as weakness and pale skin due to blood loss, though this is rare.
What Causes Hemorrhoids?Experts aren’t sure what causes hemorrhoids to develop. Several factors could be to blame, including:
- straining during a bowel movement
- complications from chronic constipation
- sitting on the toilet for a long time
- a family history of hemorrhoids
You’re also more likely to develop hemorrhoids if you’re pregnant. When the uterus enlarges, it presses on the vein in the colon causing it to bulge.
How Are Hemorrhoids Diagnosed?A visual examination of your anus may be enough to diagnose hemorrhoids. To confirm the diagnosis, your doctor may wish to do a different examination to check for any abnormalities within the anus. This check is known as a digital rectal exam. During this exam, your doctor inserts a gloved and lubricated finger into your rectum. If they feel anything abnormal, they may order an additional test called a sigmoidoscopy.
A sigmoidoscopy involves your doctor using a small camera to diagnose an internal hemorrhoid. This small fiber-optic camera, called a sigmoidoscope, fits into a small tube and then inserts into your rectum. From this test, your doctor gets a clear view of the inside of your rectum so that they can examine the hemorrhoid up close.
Can You Prevent Hemorrhoids?
What you eat and drink makes a difference. The things that help you avoid hemorrhoids are also good for the rest of your body. Eat more fiber. A good way to get it is from plant foods — vegetables, fruits, whole grains, nuts, seeds, beans, and legumes. Most Americans need more fiber, and foods are the best sources.
Stay hydrated. If you don’t, you may strain during a bowel movement and make hard stools, which further irritate the swollen veins. Drink water, and remember that you also get H2O from foods such as fruits and vegetables.
What Are the Treatment Options for Hemorrhoids?Treatment for hemorrhoids can occur at home or at a doctor’s office.
Pain Relief
To minimize pain, soak in a warm tub of water for at least 10 minutes every day. You can also sit on a warm water bottle to relieve the pain of external hemorrhoids. If the pain is too much to bear, you can use an over-the-counter medicated suppository, ointment, or cream to relieve the burning and itching.
Dietary Fiber
Home treatment can also include increasing your dietary fiber intake. Consuming foods that are high in dietary fiber can minimize the risk of developing hemorrhoids in the future.
Good dietary fiber sources include:
- whole wheat
- brown rice
- oatmeal
- pears
- carrots
- buckwheat
- bran
Dietary fiber helps create bulk in the intestines, which softens the stool, making it easier to pass.
If you’re constipated, you can also use an over-the-counter fiber supplement to help soften your stool.
Medical Procedures
If home treatments aren’t helping your case of hemorrhoids, your doctor might recommend getting a rubber band ligation. This procedure involves the doctor cutting off the circulation of the hemorrhoid by placing a rubber band around it. This causes loss of circulation to the hemorrhoid, forcing it to shrink. You shouldn’t try this at home, however.
If rubber band ligation isn’t an option in your case, your doctor can inject a chemical into the blood vessel directly. This causes the hemorrhoid to reduce in size. This treatment is known as injection therapy or sclerotherapy.
Treatments for hemorrhoids
In the majority of cases the patient can take some simple measures which will alleviate symptoms while the problem gets better on its own. However, medicines and even surgery may sometimes be needed.
Medicines
Most hemorrhoid medicines are OTC (over-the-counter); this means you do not need a doctor’s prescription to get them. They include ointments, pads or suppositories. Such active ingredients as hydrocortisone and witch hazel are known to relieve itching and pain. These medicines should not be used for more than about seven days (unless your doctor has told you otherwise).
Simple incisions
Your doctor may carry out a simple incision if a clot has formed around an external hemorrhoid. These incisions are usually effective. More continuous bleeding may require rubber band ligation, sclerotherapy (injection) or coagulation.
Surgery to treat hemorrhoids

Specialist ultrasonic device for hemorrhoid surgery.
Surgery is recommended if the patient has not benefited from the simple procedures, or if the hemorrhoids are very large. In some cases the patient may go home straight after the procedure, while in others they may have to be hospitalized. Surgery may involve hemorrhoidectomy or stapling.
The method shown on the right is a gentle method of hemorrhoidal ligation (HAL: Hemorrhoidal Artery Ligation, or RAR: Recto Anal Repair). It locates the main branch of the artery by means ofultrasound loops, with a curved needle tightly threading around the artery and pulling it together. This is called a minimally invasive treatment method and is described as being painless.
What you can do on your own
There are things you can do to relieve the symptoms. Bear in mind that they will not eliminate the hemorrhoids.
- Topical creams and ointments – you can apply an OTC cream or suppository which contains hydrocortisone. There are also pads which contain witch hazel, or a topical numbing agent
- Bathing the affected area – bathe gently with warm water. Do not use soap if you think it will make the problem worse. Dry the area gently with a hair drier after bathing
- Ice packs and cold compresses – if you apply these to the affected area it may help with the swelling
- Sitz bath. Use warm water – the sitz bath is placed over the toilet. Some pharmacies sell them
- Use moist towelletes – dry toilet paper may aggravate the problem
- Analgesics – some painkillers, such as aspirin, ibuprofen and paracetamols (Tylenol) may alleviate the pain and discomfort.
Preventing hemorrhoids
If your stools are always soft your chances of developing hemorrhoids are greatly reduced. You can help prevent hemorrhoids in the following ways:

Including plenty of fruits and vegetables in your diet will help keep your stools soft.
- Nutrition: if you eat lots of fruits and vegetables, as well as whole grains, your stools will nearly always be soft. If you drink plenty of fluids your stools are more likely to be soft (this does not include alcohol)
- Straining: when you go to the toilet try not to strain or hold your breath, as this creates pressure in the veins in the lower rectum
- Go when you need to: if you have the urge to go to the toilet, go. Do not wait. The longer you wait, the drier the stools will be
- Be physically active: physical inactivity, sitting or standing still for long periods puts pressure on the veins
- Keep your bodyweight down: obesity an overweight significantly raise a person’s risk of having hemorrhoids.






